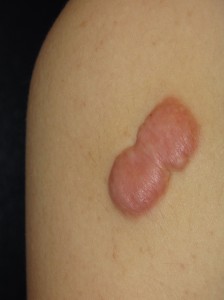
Keloids are a special type of scar that are aesthetically displeasing, often difficult to treat and can be associated with symptoms such as pain, burning, itching and stiffness. They are elevated above the surrounding skin, extend beyond the original margins of a wound or surgery site, do not regress spontaneously with time, are very firm and have a high rate of recurrence. They should not be confused with run of the mill wide but flat scars or slightly elevated ones that are thick (hypertrophic scars).
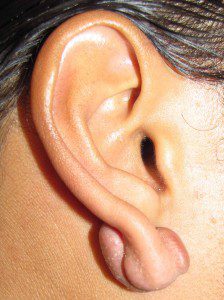
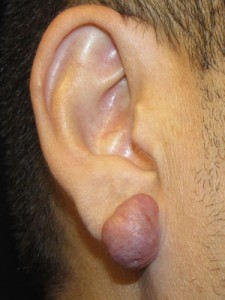
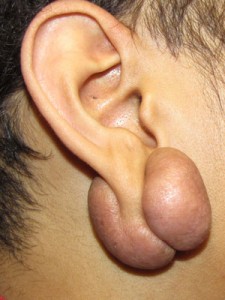
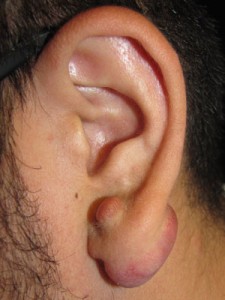
- Keloid of earlobe
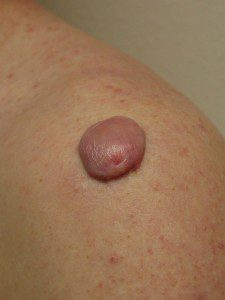
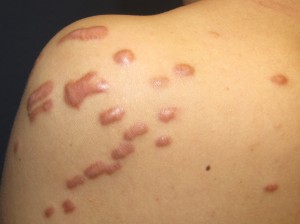
- Keloid of shoulder
There are several common risk factors that predispose individuals to develop keloids but their formation is not inevitable. Conversely though less frequently, some people can form them who seemingly don’t have any clear cut predisposition.
Who are those individuals at greater risk?
People who are dark complected (especially blacks and those of Hispanic descent), are less than 30 years old, have/had burns or ear piercings, and surgery or skin injuries to the sternum, upper arms and shoulders.
A variety of modalities and approaches have been employed for the treatment of keloids including surgical excision, steroid injections, pressure dressings, topical silicone gel sheeting, pulsed dye laser, radiation treatments and intralesional injections of chemotherapy agents. Combination therapy will often lead to better results along with a lower risk of long term recurrence.
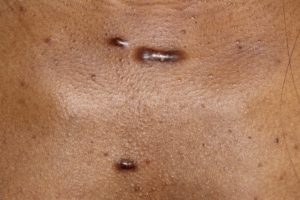
- Before
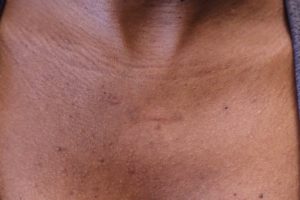
- After
Treatment by precise monthly steroid injections along with topical silicone gel sheeting.
Unless the growth is very small, my typical recommendation is for surgical excision along with repeated injections of a low dose steroid in the area and close monitoring over 1 – 2 years. Topical silicone gel strips and/or silicone gel are virtually always used in the postoperative period to help obtain the best possible outcome.
The size, location, complexity and configuration of the keloid as well as other factors will determine whether the plastic surgery treatment will be performed in the office under local anesthesia or in the outpatient center under local, sedation or even general anesthesia.
Keloids of the Earlobe and Ear
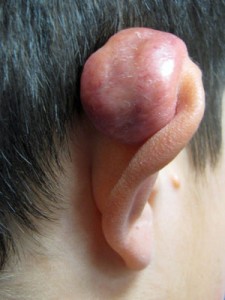
- Large Keloid of the Ear
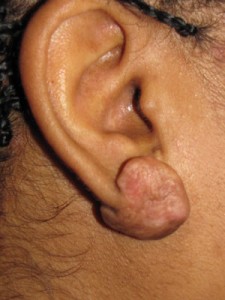
- Keloid of the Earlobe
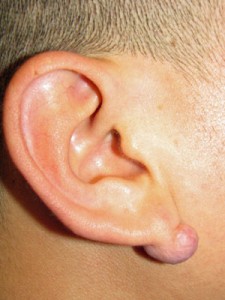
- Keloid of the Earlobe
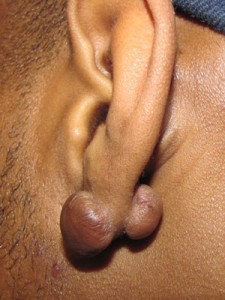
- Keloid of the Earlobe
- Keloid of the Earlobe
- Keloid of the Earlobe
- Keloid of the Earlobe
Keloids of the Face
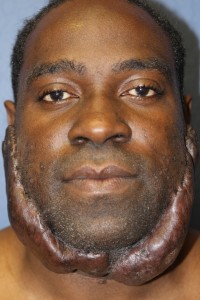
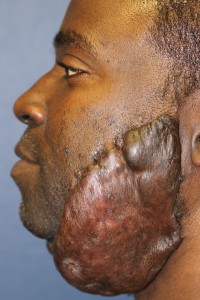
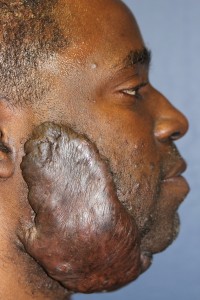
- Massive keloid of the face and neck
- Massive keloid of the face and neck
- Massive keloid of the face and neck
Keloids of the Body
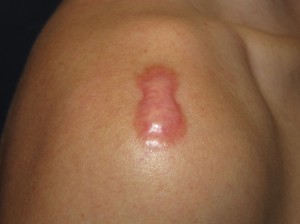
- Keloid of the Shoulder
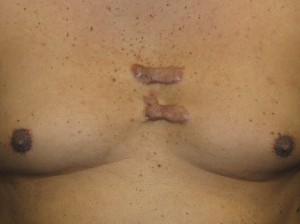
- Keloid of Chest
- Keloid of upper arm
- Keloid of the Shoulder
*Individual Results May Vary