What are Skin Cancers?
Skin cancers are abnormal, malignant growths that can involve various layers of the skin, though they most commonly originate in the very top layer called the epidermis. Because they are usually quite visible, they can be detected and treated at an earlier stage and a smaller size.
The predominant cause of the most common types of skin cancers is from excessive sun exposure. The energy of the sun’s ultraviolet rays inflicts damage to the DNA of the skin’s cells which can ultimately lead to malignant transformation. The effects are cumulative which means that a previous personal history of unprotected sun exposure will add up to an increased risk. Other factors implicated in the development of these cancers include smoking, chemicals, tobacco, and genetics.
Darker-complected individuals generally have a lower risk of developing the more common types of skin cancers. Factors which increase an individual’s susceptibility include those with a compromised immune system from immunosuppressive drugs (such as for cancer treatment, AIDS, or for transplants), advanced diabetes, and previous radiation treatments or excessive exposure.
“Just wanted to tell you how much we appreciate you and all that you do. You and your incredible staff are amazing! From our first visit, you made us feel very comfortable at a most terrifying time of our lives. The word cancer does truly make you see things in a different light.
You are blessed with a delightful sense of humor and our fondest wish is that you keep it and spread it around every chance you get.”
-L.R. Plastic Surgery Patient, Scottsdale AZ
Types of Skin Cancer
The three most common skin cancers treated include basal cell carcinoma, squamous cell carcinoma, and malignant melanoma. The basal and squamous cell carcinomas typically grow locally, rarely spread elsewhere and are “easily” curable virtually all the time, even when very large. In contrast, malignant melanomas can look fairly innocuous and be only millimeters in size yet be lethal – by metastasizing throughout the body.
Basal Cell Carcinoma
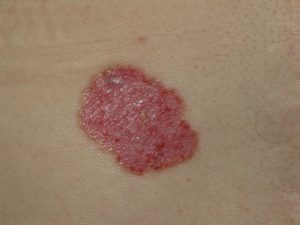
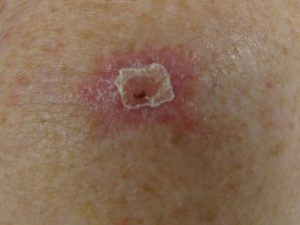
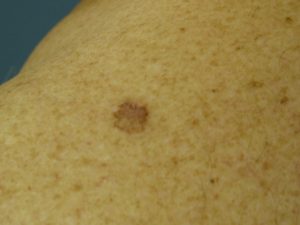
Basal cell carcinomas are the most common form of skin cancer, the slowest growing and the least aggressive – virtually never spreading elsewhere. They are often being present for several months to a year or more before becoming more noticeable. Their appearance can be that of a non-healing sore, a reddish patch or a waxy growth with an elevated margin and indentation centrally that may be ulcerated, obtaining what may look like an open sore. Rarely are they pigmented.
Squamous Cell Carcinoma
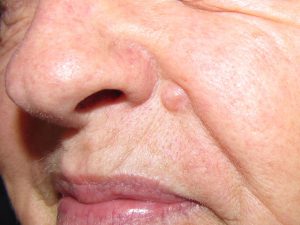
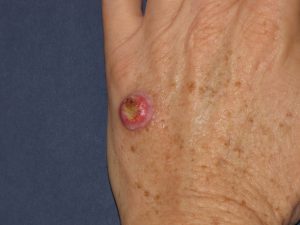
Squamous cell carcinomas often grow faster and to larger sizes than the average basal cell carcinoma but also rarely spread elsewhere. They may appear as a non-descript scaly read patch, a warty growth, an open sore, or a growth with elevated margins and central ulceration. These may actually bleed if significantly traumatized.
Melanoma
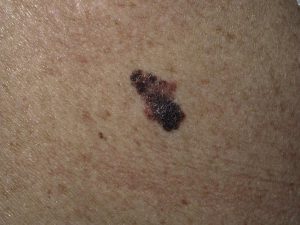
Malignant melanoma is by far the most lethal type of skin cancer and can spread elsewhere, though when it occurs on the face it often acts less aggressively. Melanomas can occur anywhere on the body including in areas not exposed to the sun and can arise from previously existing moles. The vast majority of the time they are darkly pigmented, containing different colors or shades, and are at least several millimeters in size with irregular borders.
The prognosis following treatment for a malignant melanoma is based on two factors that relate to the depth (thickness) of its growth and not its horizontal size. A small tumor that extends to a depth of as little as 3 – 4 millimeters can be associated with a high mortality rate, whereas one that is situated solely in the top layer of skin (known as a malignant melanoma in situ) can be a centimeter or more in horizontal size yet be completely curable with local surgery alone.
Diagnosis of Skin Cancers
If you have a growth or mole that looks abnormal, has changed, or is concerning you, Dr. Steven Turkeltaub recommends that you seek the assistance of a well-trained, reputable dermatologist or your primary care doctor for a diagnosis. It is advisable to seek such advice sooner rather than later as the results including the prognosis can be adversely affected if you wait longer than necessary. They may perform a biopsy if deemed warranted.
Treatment of Skin Cancers
Your dermatologist may decide to treat many skin lesions including pre-malignant ones and some skin cancers by any of a variety of methods that he or she deems appropriate. They will often elect to refer you to Dr. Turkeltaub for several reasons:
- They would like a plastic surgeon to both remove the skin cancer and repair the defect for any number of reasons.
- They would like the expertise of a plastic surgeon to reconstruct the defect created by their removal of the skin cancer (usually employing a technique called Moh’s micrographic surgery). This is usually performed as a pre-scheduled 2 stage approach.
- You request the involvement of a plastic surgeon.
At your consultation, Dr. Turkeltaub will assess the skin cancer and determine what the best treatment options will be for you, including for the removal and closure. Basal cell and squamous cell carcinomas need just a small margin of uninvolved tissue around them in order to obtain their complete removal. On the other hand, excision of malignant melanomas require minimum margins of at least one to two centimeters around them, which means the ultimate defect size, scar, and contour changes can be quite substantial and noticeable.
Your surgery would be performed at an outpatient center either under local anesthesia, with sedation (twilight anesthesia), or under general anesthesia depending on personal choice and what would be most appropriate and comfortable for you.
Closure of your wound following the tumor removal is typically performed employing one of the following three methods:
- Direct closure. Here, the wound is configured to allow for the best reconstructive/aesthetic outcome and the skin margins are then brought together and surgically repaired.
- Local flap. Surrounding tissue is recruited to facilitate wound closure.
- Skin graft (full thickness or partial/split thickness). Skin is taken from elsewhere to reconstruct the defect.
Dr. Turkeltaub will discuss with you the most relevant options for your situation including the pros and cons and the potential risks and complications.
Scheduling Your Consultation
If you have a skin cancer that you would like Dr. Turkeltaub’s expertise in treating, you can contact our office to schedule your consultation. You will also need to ascertain that he is a provider for your insurance plan.
Please contact Dr. Steven H. Turkeltaub for more information, or to schedule a consultation.