About Keloids
Keloids are raised, firm and often symptomatic scars that frequently continue to grow over time. They can be painful, unsightly, deforming and even create problematic hygienic issues.
These growths are a relatively common problem that affects people of virtually all ethnic groups. However, they are more frequently seen in those individuals who are darker complected such as of African, Asian and Hispanic descent. The risk of developing a keloid is seven times higher in blacks as compared to whites. A strong family history of these has been seen in around one third of cases.
Keloid Treatment Options
There are a variety of options available that can be employed in the treatment of keloids. The more “mainstream” approaches include:
• Corticosteroid injections (Kenalog®)
• Topical silicone gel or silicone sheeting
• Cryotherapy (cold)
• Laser therapy
• Localized pressure
• Surgical excision
• Radiation treatments
The approach(es) used depends on a variety of factors such as the size, number and location of the keloid(s), history of recurrence, financial issues, treatment resources and physician knowledge, preferences, experience and skills. Often, a combination of modalities is used to help maximize long term success.
Keloids in some areas of the body are more likely to respond well to appropriate treatment, both short and long term, as compared to other areas. In general, earlobes can do well whereas the chest and shoulders not so much. Regardless, even using the most comprehensive treatments of keloids, they still can recur no matter their location.
Factors Affect Success or Failure in the Treatment of Keloids
A very common issue that I have seen over the years in patients who have consulted me regarding the recurrence of their keloid(s) is that they had either not been treated adequately or fully by their initial treating physician or were not compliant in their treatment regimen including missing follow up appointments or not following up at all. Exacerbating this is that all too often, once there was a recurrence, the patient waited far too long before seeking re-treatment. The consequences of this is that when they do finally present for treatment of their recurrent keloid, its size was often far in excess of what it had been at the time of their initial treatment.
Illustrative Case of Massive Recurrent Keloid
The following patient of mine presenting with a recurrent keloid perfectly illustrates many of these common keloid issues:
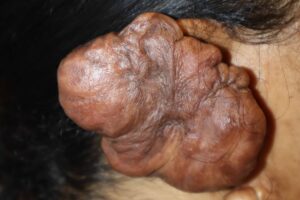
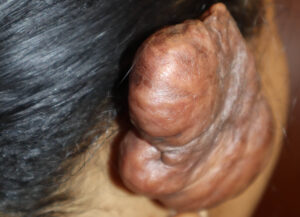
This 32 year old black female presented with a recurrent keloid of the right ear and cheek. These had been treated several years previously with surgery but there was little follow-up. Both started regrowing but she ignored seeking any treatment until they became massive in size – far larger than when she had initially sought treatment. There was also a strong family history of developing keloids and having recurrences.
On her examination, the keloid of the ear was noted to involve much of the upper half of the ear though its growth visually covered nearly the entire ear when seen from the side. It measured 3 x 2.5 inches in size.
Given all this information, nothing short of aggressive and thorough treatment would likely be effective. Therefore, my recommendation was for complete surgical excision, complex reconstruction, Kenalog® injections and immediate postoperative radiation treatments. She would then be followed up closely in the office for at least one and a half to two years to monitor for any recurrence and then aggressively treat if any recurrence was detected.
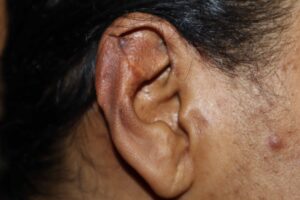
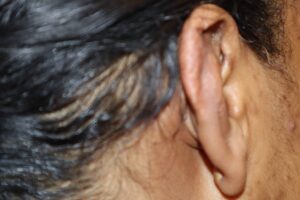
Patient agreed and had the full treatment including surgery along with Kenalog® injection at the same time followed by a course of postoperative radiation treatments. She had been followed closely postoperatively and did not show any signs of recurrence.
The Bottom Line
There are so many variables that can affect the results of treatment for keloids. However, success can be maximized by pursuing a prudent and appropriate treatment plan, following the instructions of the treating surgeon/physician, closely monitoring for any recurrence and seeking treatment ASAP if any recurrence is detected or suspected.
Steven H. Turkeltaub, M.D. P.C.
Scottsdale and Phoenix, Arizona