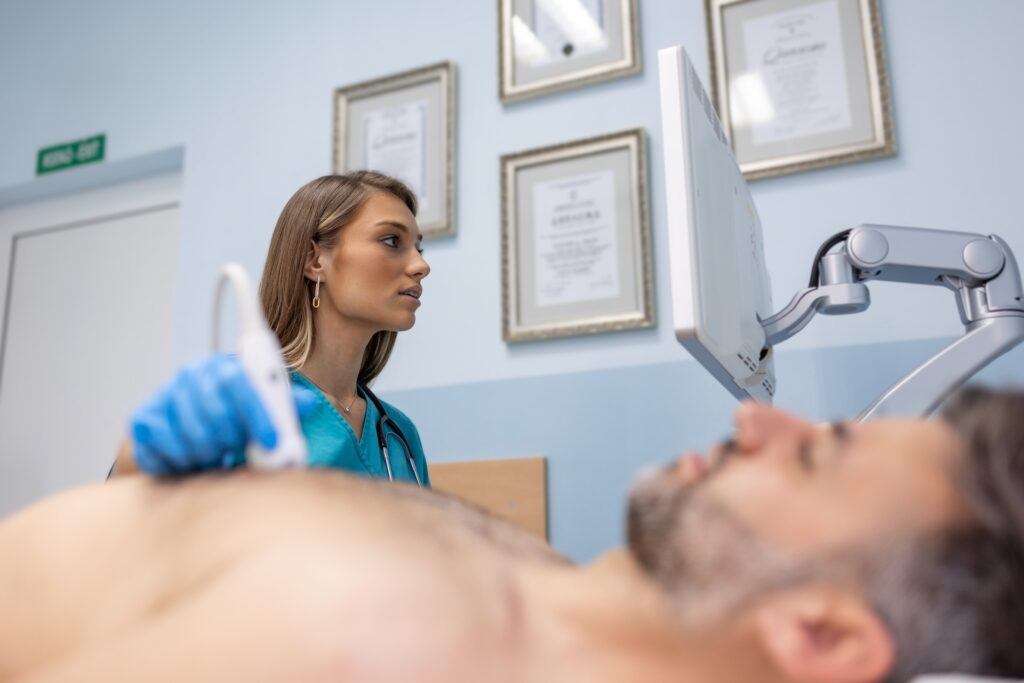
Chest ultrasound
For many transmasculine (FTM) and gender nonbinary (FTN) individuals, gender-affirming top surgery is a powerful step. By reshaping the chest and removing breast tissue, top surgery can significantly reduce or eliminate gender dysphoria and improve the quality of life.
It is important to realize that in all top surgery procedures there is still some breast tissue remaining – it not totally removed as in mastectomies done for the treatment of breast cancer. As a result, there still is a risk for the development of breast cancer
No matter how small it may be, this risk is not zero.
Consequently, you will still need to screen for breast cancer after FTM or FTN top surgery.
Why Breast Cancer Risk Still Exists After Top Surgery
Breast tissue is always left behind
No form of gender-affirming top surgery removes all the breast tissue as this is absolutely not necessary or indicated for a non-cancerous procedure. If all this tissue were to be removed, the results would be deforming, abnormal and aesthetically poor.
This would be trading one nightmare for another, in essence.
Because breast cancer arises from breast tissue, the presence of any remaining tissue means there is still a lifelong risk — even though that risk is significantly reduced compared to individuals who have not had top surgery.
How much does top surgery reduce risk?
Top surgery tremendously lowers the amount of breast tissue present and, therefore, substantially reduces breast cancer risk. However, it does not eliminate it. There have been documented cases of breast cancer developing in transmasculine and gender nonbinary individuals years after top surgery including cases where cancer arose in residual tissue along the chest wall or near surgical scars.
Long-term data on breast cancer rates in FTM and FTN individuals is still limited so most medical organizations recommend a cautious, individualized approach to screening rather than assuming that the risk is eliminated.
Factors That Influence Breast Cancer Risk After Top Surgery
Although all individuals retain some breast tissue after surgery, certain factors may increase overall risk:
- Family history of breast cancer
- Genetic mutations, such as BRCA1 or BRCA2
- Personal history of breast cancer or high-risk breast lesions
- Extent and pattern of residual breast tissue
- Age
- Duration of estrogen exposure prior to surgery
- Testosterone reduces breast cancer risk but does not eliminate it
Who Should Be Screened After Top Surgery?
Because all individuals retain breast tissue after top surgery, the key question is not whether screening is needed, but what type of screening is appropriate.
Screening decisions should be based on:
- Individual risk factors
- Type of surgery performed
- Amount and distribution of remaining tissue
- Personal and family medical history
Screening is especially important if you:
- Have a strong family history of breast cancer
- Have a known genetic mutation linked to breast cancer
- Have had breast cancer in the past
- Notice new or persistent symptoms, such as:
- A lump or firm area in the chest wall
- Skin changes or dimpling
- Nipple discharge or inversion
- Swelling near the armpit
- Unexplained chest wall pain
Even individuals without high-risk factors should remain chest-aware and seek evaluation for any changes.
How Is Breast Cancer Screening Done After Top Surgery?
Traditional mammograms are not possible or effective after FTM or FTN mastectomies but can be done in those individuals who have had gender affirming breast reductions – commonly requested in androgynous individuals.
The following are other imaging options that are commonly used:
Ultrasound
- Frequently the first-line imaging method
- Effective for evaluating lumps, pain or localized changes
- Well-suited for minimal or redistributed breast tissue
- Significantly less costly than an MRI
Breast MRI
- Often recommended for individuals at higher risk
- Useful when anatomy is complex after surgery
- Highly sensitive for detecting abnormalities
A healthcare provider can determine the most appropriate imaging approach based on anatomy and risk profile.
Chest Self-Awareness After Top Surgery
Because breast tissue remains after surgery, ongoing chest self-awareness is essential.
Rather than traditional breast self-exams, clinicians often recommend becoming familiar with your post-surgical chest by:
- Feeling along scars, the chest wall and underarms
- Noticing new lumps, firmness or asymmetry
- Watching for skin or nipple changes
- Paying attention to persistent discomfort or swelling
Any new or concerning change should be evaluated — even many years after surgery.
Key Points to Remember
- Breast tissue is always left behind after top surgery
- Breast cancer risk is lower or low, but not zero
- Screening should be individualized and anatomy-based
- Ultrasound and MRI are commonly used after surgery
- Chest self-awareness is a lifelong practice
- Affirming, informed healthcare supports better outcomes
Final Thoughts
Top surgery is a life-affirming procedure and protecting your long-term health is part of honoring that choice. Understanding that breast tissue remains, staying aware of changes and engaging in appropriate screening allows FTM and FTN individuals to take proactive, empowered steps in their care.
Steven H. Turkeltaub, M.D. P.C.
Scottsdale and Phoenix, Arizona