For around a century, some form of mastectomy, which is the total removal of the breast tissue, has been employed in the treatment of breast cancer. Originally, this was the highly deforming and extensive radical mastectomy as first proposed by William Halsted in 1894. This was later replaced by the modified radical mastectomy which was significantly less deforming but still aesthetically and emotionally devastating to many women. First introduced in the late 1940’s, it became quite popular in the 1970’s.
With advancements in diagnostics and non-surgical breast cancer treatments, operative techniques have continued to evolve into approaches that are less deforming, leaving more breast elements. This include skin sparing mastectomies where no skin at all is removed except for the nipple-areola complexes. With nipple sparing mastectomies, not only all the skin but also the nipple-areola complexes are preserved.
Lumpectomies take this even further – removing only the tumor and a small margin of normal tissue and preserving the remaining breast tissue, all the skin and the nipple-areola complexes. Typically, this approach is also combined with radiation treatments and is generally classified as breast conservation therapy (BCT).
By removing only the minimum amount of tissue necessary to treat the breast cancer, patients who have undergone a lumpectomy are left with a substantial amount of normal breast tissue which can help facilitate superior reconstructive results. The various reconstruction techniques that are associated with this breast conservation therapy are classified as oncoplastic breast reconstruction.
The outcomes from these procedures can be far better and more natural as compared to those obtained after any of the various mastectomies techniques. In fact, several studies has shown a better quality of life including increased self-esteem and improved body image and sexuality with this approach as compared to outcomes associated with mastectomies and standard reconstructions. This should not surprising whatsoever because with mastectomies, all the breast tissue is removed as compared to only a small amount with lumpectomies.
What oncoplastic reconstructive techniques all have in common is the usage of the remaining available breast and surrounding tissues. There is no usage of breast implants or tissue expanders.
The procedures associated with this reconstruction can be grouped into three general categories. These include:
1. Contouring of the remaining breast tissue. With this approach, the breast tissue remaining after the tumor removal is mobilized to fill the defect and facilitate a more normal appearing breast. This also can involve contouring of the breast skin and repositioning of the nipple-areola complex when indicated.
2. Breast lift or breast reduction. If the breast is large and/or droopy, either a breast reduction or a mastopexy is performed in order to obtain a quality reconstruction. This is performed in addition to the breast tissue mobilization (as described above) to address the breast contour defect. Typically, this also involves a symmetry procedure on the other breast (see photos).
3. Local flaps. Though not used very often, tissue can be brought in from surrounding areas to help contour the remaining breast and help fill out areas that are difficult to address otherwise.
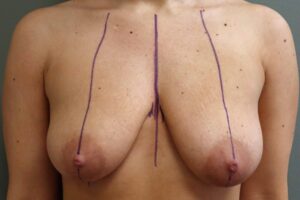
Before lumpectomy and lymph node sampling of the left breast
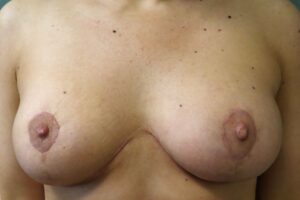
2 months after oncoplastic breast reconstruction with mastopexies
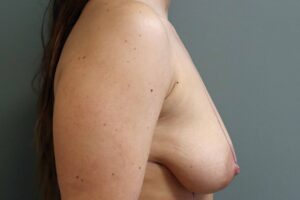
Before – side view
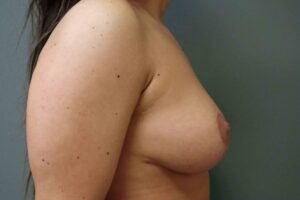
After – side view
Just because a lumpectomy is being performed in conjunction with breast conservation therapy does not mean that every patient undergoing this type of surgery is an appropriate candidate for this oncoplastic breast reconstruction. There are many factors and issues that should be evaluated before one can be considered as a good candidate for this approach. All of this can be discussed with your cancer surgeon and plastic surgeon, where appropriate.
For more information on breast reconstruction or to schedule a consultation, you can contact our office at (480) 451-3000 or by email.
Steven H Turkeltaub, MD
Scottsdale and Phoenix
